Bursitis Of The Foot Bursa Removal Complications
Overview
Bursae (two or more bursa) are small, fluid-filled sacs that cushion the bones, tendons and muscles surrounding your joints. They contain a lubricating fluid that reduces friction, allowing tissues in the body to glide past each other smoothly. Imagine the bursa as a protective layer that helps keep a tendon or muscle from fraying or getting aggravated as it eases over a bone or around a corner. Bursitis is a condition that occurs when a bursa becomes inflamed: irritated, red and filled with more fluid than normal.
Causes
Bursitis may be the result of a direct injury to the heel, such as during a car accident, sport-related accident, or fall that causes a forceful impact or abnormal twisting of the foot. It can also occur due to repetitive use, misuse, or overuse, such as seen in athletic over-training. Excessive pressure over the subcutaneous calcaneal bursa, such from wearing shoes that are tight or fit poorly, can also be a causative factor. Septic bursitis occurs secondary to an infection. The infection may occasionally be systemic, but is most often a localized infection from a subcutaneous heel wound that leaks into the underlying bursa. Other risk factors include any of the following, existing Achilles tendinitis, existing Haglund’s deformity, the natural degenerative processes of aging, improper stretching prior to exercise, anatomical differences in the lower extremities that impacts gait, having deformed joints.
Symptoms
Pain at the back of the heel at the attachment site of the Achilles tendon when running. Pain on palpation of the back of the heel or bottom of heel. Pain when standing on tiptoes. Swelling and redness at the back and bottom of the heel.
Diagnosis
When you suspect you have retrocalcaneal bursitis, your foot doctor will begin by taking a complete history of the condition. A physical exam will also be performed. X-rays are usually taken on the first visit as well to determine the shape of the heel bone, joint alignment in the rearfoot, and to look for calcium deposits in the Achilles tendon. The history, exam and x-rays may sufficient for your foot surgeon to get an idea of the treatment that will be required. In some cases, it may be necessary to get an ultrasound or MRI to further evaluate the Achilles tendon or its associated bursa. While calcium deposits can show up on xray, the inflammation in the tendon and bursa will show up much better on ultrasound and MRI. The results of these tests can usually be explained on the first visit. You can then have a full understanding of how the problem started, what you can do to treat prevent it from getting worse/ You will also know which treatment will be most helpful in making your heel pain go away.
Non Surgical Treatment
Other than rest, once the diagnosis of heel bursitis (Achilles bursitis, Retrocalcaneal bursitis) has been confirmed then your treating doctor will either generally recommend one or more of the following, Pain killers. Non steroid anti-inflammatory medication. A cortisone steroid injection. Surgery in extreme cases. Whilst the above may be beneficial for some people, others unfortunately will not be suitable for such heel bursitis treatments. This may be for several reasons such as having already tried these medications with little to no benefit or not being able to take these type of medications due to pre-existing medical conditions or alternatively some individuals may just prefer to avoid painful injections or strong medications and instead use a natural heel bursitis treatment.
Surgical Treatment
Surgery to remove the damaged bursa may be performed in extreme cases. If the bursitis is caused by an infection, then additional treatment is needed. Septic bursitis is caused by the presence of a pus-forming organism, usually staphylococcus aureus. This is confirmed by examining a sample of the fluid in the bursa and requires treatment with antibiotics taken by mouth, injected into a muscle or into a vein (intravenously). The bursa will also need to be drained by needle two or three times over the first week of treatment. When a patient has such a serious infection, there may be underlying causes. There could be undiscovered diabetes, or an inefficient immune system caused by human immunodeficiency virus infection (HIV).
 Overview
Overview Symptoms
Symptoms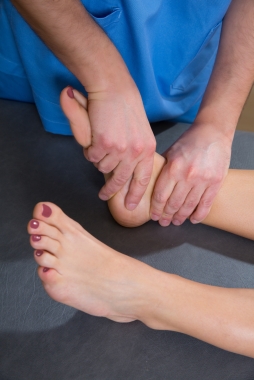 Prevention
Prevention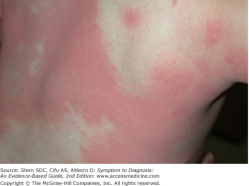 Overview
Overview Symptoms
Symptoms Prevention
Prevention
 Achilles Tendonitis or achilles tendinopathy which is probably a more accurate term is an overuse injury causing pain, inflammation and or degeneration of the thick achilles tendon at the back of the ankle. The term achilles tendinopathy is probably a better term to describe the range of conditions that can cause achilles tendon pain. Achilles tendonitis can be either acute or chronic. Acute achilles tendonitis is usually more painful and of recent onset. Chronic achilles tendonitis will have come on gradually and over weeks, not necessarily preventing activity.
Achilles Tendonitis or achilles tendinopathy which is probably a more accurate term is an overuse injury causing pain, inflammation and or degeneration of the thick achilles tendon at the back of the ankle. The term achilles tendinopathy is probably a better term to describe the range of conditions that can cause achilles tendon pain. Achilles tendonitis can be either acute or chronic. Acute achilles tendonitis is usually more painful and of recent onset. Chronic achilles tendonitis will have come on gradually and over weeks, not necessarily preventing activity.

